While there are a lot of things I love about going to the Myelo Clinic at C.S. Mott Children’s Hospital, such as seeing most of the practitioners all in one shot, there are things that are overwhelming about the clinic, such as seeing most of the practitioners all in one shot. Even though I had a lot of questions for the various doctors going into today, I didn’t really think too much about what the answers might all lead to. I kind of knew a few things to expect, but overall as I started to jot down all the follow-ups, it quickly felt overwhelming. We left with these marching orders:
– new AFOs
– a mobile stander
– Opthamology referral
– sleep study referral
– helmet #2
My Aunt MJ reminds me often how I once asked her, “How do you do it? How do you get up every morning and keep doing all this?” At the time she was helping to carry the weight of three very close family members fighting cancer battles. She turned the question on me after Colten was born. Her answer and my answer are the same: We do it because we love these people. We do it because they need us. We do it because we want the best for those people.
It’s easy to look on from the outside and think, “I could never do that.” “It takes a special person to have a special needs child.” YES YOU CAN, and NO IT DOES NOT. If you were handed a child that needed extra care or a spouse that needed extra care, you too would hopefully step up and provide whatever you could for them. Because you love them and want the best for them. That’s what we do. We are not any different or more or less special than any of you (and frankly, if we were special, I can think of about 1,000 things I would define as special that I would prefer over Spina Bifida, such as winning the Lotto – those people are special, right?!) It can and does happen to anyone and we aren’t special. We have to make a choice every day about our children, special needs or not. Some times we make great choices and sometimes we wish we could get a do-over. Every parent and every child experiences this. We have special circumstances, we are not special people. You also have special circumstances and everyone handles and interprets those differently.
I know this from two very memorable bits of communication over the last year or so. The one was with my cousin Jason. After finding out about Colten’s medical complications, he emailed me to reach out and give support. It is also his daughter battling cancer. I cannot fathom the fear, helplessness and effort it takes to support a child battling cancer and the thought of it overwhelms me and makes Spina Bifida feel like a walk in the park. In an email that blew me away, he expressed a somewhat opposite thought: he could not fathom the energy it would take to support a child with lifelong medical needs and permanent disabilities. Cancer, to him, was something that they could fight, win and get past. It’s all about perspective. The second conversation was between Richard and another dad in the NICU at Mott. This father was there with his son who would require roughly 10 extensive surgeries over the first year of his life and would spend at least the first six months of his little life in the NICU. Richard felt for the family and listened as the dad shared all the medical complications this child was born with. When the dad was done, he asked Richard about Colten. The look on the man’s face when he realized Colten would probably not walk independently and might need a wheelchair to get around, shocked Richard. Here this man was waiting while his son grew strong enough for all the surgeries and he seemed more bothered by our situation. His comment was that at least once his son made it through his surgeries, he would come out the other side and lead a pretty normal life. I’m guessing with that many extensive surgeries, there’s a lot of care involved down the road, but then again, I don’t know. Either way, it’s all about perspective.
Alright, back to the details. We had a LOOONG three days of a lot of medical appointments, thus, this is a LOOONG post to recap everything. So if you don’t already have a cup of coffee or glass of wine, you might want to break for a minute and go grab that.
We started Wednesday with Colten’s slightly late 1-year checkup with his new pediatrician. Finding a doctor that had privileges at the local children’s hospital (Beaumont) and accepted both Colten’s insurance and the insurance Parker and Max are on, was, frankly, a bitch. I think we had four options throughout the entire Metro Detroit area and three were in an office 35 minutes away. I don’t recall the fourth but we went with that office. I AM SO GLAD WE DID. I randomly chose one of the doctors from the three listed and could not believe my luck! The first great impression was when the office staff called to move our appointment to a different day because the doctor had reviewed his records and wanted us to be assigned a longer appointment time so we could talk without being rushed. I greatly appreciated this and sure enough, I think her and I talked for a solid thirty minutes. She had some great questions about his past procedures and experiences, and herself having a daughter with cerebral palsy, was able to share some local therapy resources and information that would be helpful for us.
That appointment went very well. Besides upright movement – standing, steps, walking, Colten is pretty on-track for a one-year-old. She had a baseline blood test done; Colten had the typical slightly-delayed cry reaction to the finger prick – and was so adept at removing his bandaid the nurse had to double him up. His blood came back slightly low in iron and the pediatrician commented that with another child, she would recommend supplementing iron in, however, that would really just make him more constipated. That already being an issue, she didn’t feel the iron was THAT low to warrant supplementing at the risk of further constipation. She was very encouraging about continuing the high fiber diet we try to keep him on (thankfully, he LOVES prunes) and said she prefers sticking to the natural routes as well and avoiding medication when necessary. I wanted to hug her for getting all that.
After that, Colten and I went over to the Beaumont physical therapy office for his session. I talked to his PT about how we’ve continued to work with him going from a seated position to standing while up against an activity table, chair or couch. I mentioned we do most of this without braces and she was interested in seeing how he did that way so we ended up completing the whole session without them! We feel this is important to his brain mapping and bodily mechanics. We have struggled with adding braces to his legs, even though they’re just for therapy, because when you add bracing and support, the body doesn’t have to work as hard with that particular body part. If it doesn’t have to work, it eventually may NOT work very well. I’m too lazy to go look for the research right now but it is out there. This can be seen when someone has an arm or leg in a cast for an extended part of time. When out of the cast, rarely does the patient just go back to normal. There is some level of therapy involved in order to regain range of motion and strength. Often, the body part not only weakens and stiffens, but shrivels up a bit. So we have been very adamant that we want Colten to use his body without bracing as often as he can. It’s not because we’re mean or denying the fact that he needs the assistance, we just realize that bracing is complicated and can be uncomfortable and can even get in the way (he struggles to crawl when his leg braces are on). We only use his leg braces during land sessions of PT (roughly 2x/month), and then about half the time when purposefully working on some movement at home (so another 2-3 times each week). So Holly worked this session without them. He did good! It took more effort on her part to get his feet to stay aligned enough to help support him but it was a great experience for his legs and feet and we are thankful she is working so well with him.
Day 2 – down in Ann Arbor. In case you’re a new follower of the blog, Myelo Clinic is when the Children’s Hospital brings in a large group of Myelo kids all on one day. They put each family in a room and the doctors move from room to room.
The first team to come see Colten was urology. Since we just had his testing done (ultrasound and CMG) and his bladder is emptying “good enough” for now and his kidneys are not being damaged by the reflux and he hasn’t had ANY UTIs (woohoo!), they technically cleared us for one year. This is kind of false though, as we have a post-op appointment in about 3 weeks, and he has part 2 of surgery in about 5 months, which will require another post-op appointment after that. But, this means that unless there’s a drastic change in bladder function or infections, we do not have to catheterize him yet (very, very common among people with Spina Bifida).
Next up was social work. I’m not entirely sure why they are part of this but sometimes have been very helpful with insurance information, family support resources, hospital resources, etc… Well, that’s probably why they’re a part of this clinic then!
PM&R (Physical Medicine & Rehabilitation) was next. This is always an overwhelming group and they are the ones that, besides urology, usually have the most going on with each patient. They are in charge of all therapies (PT, OT, speech, etc…) and all equipment needs (special strollers, braces, orthotics, wheelchairs, adaptive equipment of any kind). I had a lot of questions they were able to answer so as overwhelming as that session became, it was helpful and productive. First up was sleep issues. Knowing that many children with Spina Bifida and other low-tone conditions have sleep apnea, we are just a little concerned about Colten’s sleep changes. Up through about 8 months of age, this child was a miracle sleeper; we laid him down with his little blankie and he would snuggle up and just fall asleep in his bed. He would sleep all night. ALL NIGHT. It was wonderful! Then around 8 months he started moving more in his sleep and waking more at night. Sometimes just patting his butt helped lull him back to sleep, or moving him from his back to his side, which is his preferred way to sleep (hence the misshapen head). Sometimes only a bottle or some playtime would ease him back to dreamland. Our other two boys were night wakers so we didn’t think too much about it – figured that gravy train of all-night sleeping was just done. We assumed he was learning a new skill, teething, etc… Now that this has gone on for five months and he rarely seems to make any progress beyond one good night here or there, and the fact that we’ve noticed he wakes more often when on his back – almost never when on his side, and seems to struggle more with breathing when he is on his back, we figured we would present the information to the doctors and go from there. Not surprisingly, they are erring on the side of caution and ordering him a sleep study. No date on this yet but more to come later.
Our next point of concern was his left eye. This has actually, in my opinion, gotten a bit better, but the pediatrician noticed it and wanted us to address it with the PM&R team as well. It just kind of floats in sometimes. This is somewhat common in younger babies. Once they hit a year it should be stronger and not float as much so they put a referral in to Ophthalmology. We set the appointment up but it’s not until the end of January. I think I’ll have to be calling in for cancellations to get that moved up! We anticipate that they will either want to just give it more time to strengthen on its own, or they could possibly put an adhesive patch on the good eye to force the weak eye to get used more. I’m assuming this is done with great caution as we certainly wouldn’t want to weaken the good eye (recall the earlier paragraph about how casting weakens a body part?!). We’ll see. More on this later of course.
Next up was our concern about how incredibly sensitive his lower back is right around his lesion. This certainly makes sense, as there is no protective spinal bone down there like the rest of the back, to protect the spinal cord and nerves. Where his lesion is, the spinal process is missing (those bumps you feel on your back down your spine). But he lights up crying when this part is touched. Because sometimes there is a “down there” explosion, we have to clean out that area – his scar goes from his low back down right into the butt crack and the skin kind of folds and dimples so it’s easy to get stuff caught in there. This requires a good cleaning and the pressure from cleaning has certainly caused him to go to tears before. Then, boys being boys, we’ve had a few cases of tumbles where one boy’s hand or foot ends up at the lesion point. This does not make Colten happy and while we don’t want to be overly cautious and protective at every waking moment, we also don’t want to see him in that much pain. So we were advised by a couple other families in the SB community to ask the rehab doc about massage or brushing to desensitize the area, in a way. Provide it more stimulation so that it would become more comfortable with input. The occupational therapist gave us a massage technique and advised us to do that every day with vitamin E along his incision, starting with light massage and overtime, increasing the pressure he is able to withstand. So we’ll try to get right on that.
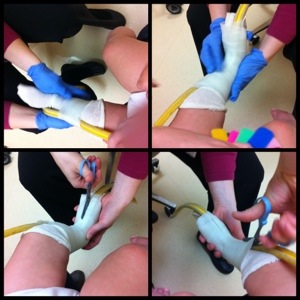
Dr. Green watched him crawl and climb up to his knees and was happy with his mobility. She put his braces on him and seeing that his toes were starting to come over the edge, recommended a new brace, this time including a strap over the front of the calf. Since he’s too big for the “sized” AFOs, they asked the orthotist to come back and fit him for custom AFOs. After they completed the rest of their clinic rounds, she came back in and did the fitting. I’m assuming this is similar to what they do for a cast: they wrapped his one leg in pre-wrap, then in wet casting material. She held his foot in alignment and allowed the cast to harden. Before putting the pre-wrap on, she had placed a rubber piece along the front of his shin and wrapped everything around that and his leg. This allowed her to easily cut the cast off after it hardened. She repeated this with his other leg and in about 15 minutes or less had both molds done for his new AFOs. Because these are custom, we had the opportunity to pick out the colored straps, padding and accessory strap. So coming to Colten’s feet soon will be dinosaur AFOs! Coincidentally, I met a mother today whose son wears AFOs too and they call his “magic boots”. I like that 🙂
Here he is getting fitted for his new braces…it will be a few weeks until he gets them.
Dr. Green also put in a script for a mobile stander. We are struggling with this a little bit for a few reasons: necessity and usability. So the reasons FOR a mobile stander, which is basically a wheelchair he stands in as opposed to sitting in (picture below), include building bone density, increasing circulation, improving digestion, enhanced cardiovascular condition, eye-level with peers, and added mobility and access. The issues we foresee with a stander are decreased lower body activity, inability to have full freedom of movement (once he is strapped in, he’s in until we take him out; he cannot bend over or get anything on the ground – only things at height level), figuring out how to make being in there worth the time for him, and where in the world we’ll use it. We’ve seen some families use it to do activities at a kids table – instead of having him sit at the table, he would be able to roll up to it and maintain the standing position instead of being seated. It takes months to get this so we’ll see how it all plays out. It’s something we’ll only use for short bouts of time and maybe not even every day.
This is a picture of the type of stander he will get:

Neurology came to visit next and all looked good. The neurosurgeon felt his shunt and fontanelle, did some testing of his lower leg, asked some questions, checked some recent medical records and felt comfortable releasing us through six months instead of three. When we’re back in six months, he wants Colten to have a quick MRI, which is similar to a regular MRI but they don’t put the little guys out entirely, just sedate them mildly. The purpose of this MRI will be to check the brain and shunt, and I’m not sure if they’ll do the lower spine but I imagine they’ll get a glance at the Chiari malformation while they’re scanning up there.
Now, for the thorn in my side. Head shape. After our last visit with the orthotist who handles Colten’s braces and helmet, we were given a weak outlook on any future changes to his skull. His head was growing up not out and in the months he had been wearing it, he had absolutely NO side to side growth at all meaning his head is still quite elongated and narrow in the back. We could either continue with the helmet and see if any changes occurred or we could be done with it. After a frustrating couple days, we decided to be done for the time being. However, his head shape has continued to be bothersome to us in a few ways. We were unsure of how the narrowing in the back would impact his Chiari malformation (we have now been told it will not impact it – yay!), we didn’t want him to have “one more thing” that was a point of possible discomfort (socially/emotionally; kids are mean and his head looks like a torpedo in the back), and we really wanted to be able to fit him into bike helmets safely – we bike ride a lot! So we figured at the least, we wanted the cranial doc (plastic surgeon) to take a look and reassure us that his head did not require surgery and that the shape is what it is – or give us further advice. Fortunately, Mott worked us into an appointment with Dr. Bachmann the same day we were in that clinic area for Myelo, so Dr. Bachmann came to see us while were waiting out the other rounds of practitioners.
Dr. Bachmann agreed his head was still very scaphocephalic (long and narrow), and we confirmed AGAIN that he was not a preemie (they seem befuddled by the fact that his head is shaped like this and he wasn’t a preemie). He talked to us about the helmet he had and said in his opinion, we do have a while longer where we can push for some progress but with a very different approach. He explained that kids with shunts do not respond like non-shunted kids to helmets and it takes a much longer time and a higher pressure to force the change. He feels the openings in the original helmet did not necessarily allow for the right area to expand and it was not tight enough front to back. He also wants him in a full helmet, whereas his original one was open on top. So, we will head back to get measured for another helmet, hopefully soon. Dr. Bachmann suggested leaving him in it 2-3 months, then re-evaluating. If we’re seeing changes, keep it on until no additional changes are seen. If we see no changes, take it off and leave it alone.
That was Thursday. We still have Friday…
Watch for Part 2! That was enough to put us to sleep for now…










Love reading about Colten’s adventures. Hugs to all!!!!!
Kate,
Your opening reflection was beautiful and challenging. Thanks for this wonderful update!
My sister started wearing glasses and an eye patch when she was 14 months old.
Forrest Gump called his leg braces “magic shoes” they were supposed to fix his back from being crooked like a question mark. Look where those shoes lead him – Purple Heart, ping pong champ, shrimpin boat captain, millionaire!
Thanks for the update and the adorable pictures breaks 🙂
Wow you guys sure have been busy with the doctors and all Coltons check-up. Really sounds like things are going mostly good. He is making so much good progress. I just love that little face and eyes, he makes me laugh whenever I see it on these postings! ha ha ha I was reading some information on the rifken stander, that looks pretty cool. maybe he is just a little young yet to get that ? I see they are really $$$. But I bet when and if the time comes he would love to learn how and be able to scoot around the house at a higher level sometimes and social activities. Also still improving his crawling skills at other times. Sorry, just thinking outloud. Wish my niece Faith had that stander if she COULD use it with her SB. I have to ask her mom about that.
He is gonna surprise you a lot this coming year, if he keeps learning as fast as last year. Happy holidays, I hope I get to see you and everyone at St Angela’s during the holiday Masses.
Kate… despite your remarks to the contrary… you guys are “special”… Special to me and a whole lot more people. I so love your updates. Hugs to all of you… aunt mj